Uterine Fibroids (Leiomyomas)
What are Fibroids?
Uterine fibroids (called leiomyomas) are a common, benign growth in the uterus, made up of muscle and connective tissue from the uterine wall.
Fibroids occur in up to 80% of women aged 50 or over and can be asymptomatic, meaning you won’t always have any symptoms or otherwise know they are there. Whilst they generally aren’t dangerous, they can cause significant discomfort and serious symptoms for some suffers.
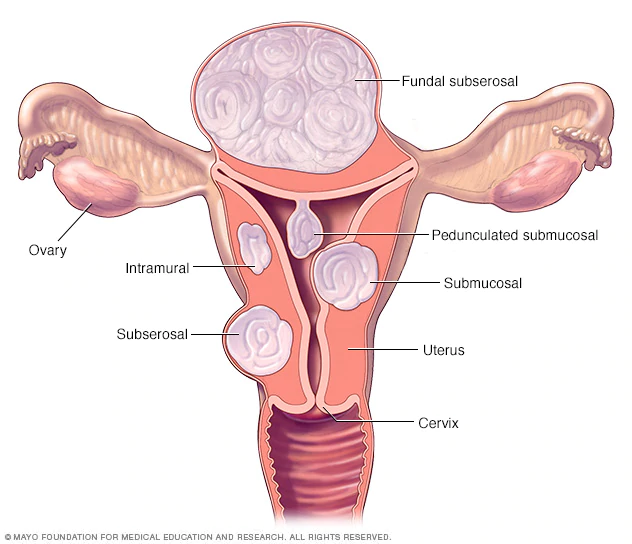
Image credit: Mayo Clinic
Fibroids can grow in a single node (that is, by itself) or in a cluster. Most clusters vary in size between 1mm and 20cm in diameter. In some extreme cases they can grow to the size of a watermelon.
Fibroids can distort the lining of the uterus, leading to heavy or abnormal bleeding, pelvic pain, and iron deficiency anaemia. Very large fibroids can also put pressure on the surrounding organs, causing pain and bloating as well as bladder problems.
There are 4 major types of fibroids:
- Intramural fibroids - these grow in the wall of the uterus itself.
- Subserosal fibroids - these are the most common type of fibroid and start as intramural before projecting outside the uterus.
- Submucosal fibroids - these fibroids are uncommon, and grow inside the uterus and project into the space where a baby grows during pregnancy.
- Pedunculated fibroids - these grow on a stalk attached to the uterus and are the least common type of fibroid.
What Causes Fibroids
We don’t know for sure what causes uterine fibroids, but we do know that some women are more likely to get them than others. Factors that can increase your risk include:
- Family history – if your mother, sister, or grandmother have fibroids, you may have a higher risk
- Pregnancy – hormone changes during pregnancy can cause fibroids to develop and grow quickly
- Obesity – obesity is a risk factor for a wide variety of health conditions, and some studies have shown that an unhealthy weight may affect the development of uterine fibroids
- Blood pressure – having a higher than average blood pressure for your age has been shown to have a relationship to uterine fibroids.
- Age – women over age 40 are much more likely to develop fibroids.
- Diet – a diet high in red meat and alcohol and low in green vegetables, fruit, and dairy may increase the risk of developing fibroids, although this is yet to be conclusively proven.
- Early-onset of puberty – some studies have found that women who entered puberty at an earlier than average age have an increased chance of developing fibroids.
What are the Symptoms of Uterine Fibroids?
If you show signs of having uterine fibroids, your GP may recommend a series of tests to determine a diagnosis. Signs to watch out for include:
- Heavy periods – you may soak through pads or tampons very quickly (within 1-2 hours)
- Passing large clots – regularly passing clots more than 2cm wide is worth mentioning to your doctor
- Tiredness – having a constantly heavy period can lead to iron deficiency anemia
- Painful periods and/or sex – fibroids can make any contractions or pressure painful, especially if they form near the cervix.
- Infertility – fibroids can impact the way the uterus functions, making it harder to conceive
- A feeling of pressure in the pelvis – this can be caused by uterine fibroids putting pressure on other organs
- Frequent urination and difficulty emptying the bladder – large fibroids may put pressure on the bladder.
- Constipation – this can happen if fibroids begin to put pressure on the colon.
- Leg or back pain – very large fibroids at the back of the uterus can put pressure on or pinch the nerves at the base of the spine.
- Incontinence – you may urinate a little when you laugh or sneeze.
For a comprehensive look into the symptoms of fibroids, be sure to read our blog: What are the Symptoms of Fibroids?
Are Uterine Fibroids Cancerous?
Uterine fibroids are a type of tumour, but they are benign (non-cancerous). Unlike cancers, they cannot spread to other parts of the body and can generally be treated in a single procedure. However, it is possible for a uterine fibroid (or leiomyoma) to develop into a malignant growth (a leiomyosarcoma). This is sometimes picked up on an MRI scan or may be signalled if a patient doesn’t respond to a uterine fibroid embolisation (UFE) or other fibroid treatment as expected.
Do Fibroids Affect Fertility?
Depending on their size and position, fibroids can make it difficult to conceive by blocking embryos from attaching to the uterine wall and may affect your ability to carry and deliver naturally. As a result, having them removed may improve your ability to become pregnant.
Studies have shown that surgical removal and embolization treatments can improve fertility outcomes. This evidence shows that there is no clear difference in the ability to conceive between patients who have undergone myomectomy and uterine fibroid embolisation, and the most ideal procedure for your case will be discussed at your consultation.
Discover more about fibroids and fertility here.
Do I Need to Have Fibroids Removed?
Even though fibroids affect about ¼ of women, only about 40% of the affected will need treatment. Since they only need medical intervention if they produce symptoms, you may not need medical intervention if your fibroids aren’t negatively affecting you or impacting your ability to do what you love.
For most women, untreated fibroids don’t cause major symptoms. However, they may continue to grow and multiply, leading to concerns such as heavy bleeding, anaemia, pelvic pain or pressure, and complications in fertility and pregnancy.
Can Exercise Shrink Fibroids?
There is an established link between exercise and the prevention of further growth of fibroids, but exercise alone cannot actually shrink existing fibroids, nor can it prevent them from developing in the first place. But that doesn't mean you shouldn't adopt a more active lifestyle to help treat your symptoms.
Exercise can reduce the hormones - estrogen and progesterone - responsible for the growth of fibroids. Regular exercise also reduces blood pressure and aids with weight loss, two more suspected causes of fibroids. Find out more about fibroids and exercise by reading our blog.
Can Diet Changes Impact Fibroids?
Yes, research has shown that certain foods can improve your symptoms, while others can worsen them or increase your risk of developing fibroids. Find out more about fibroids and diet on our blog.
How are Fibroids Diagnosed?
The first step in diagnosis is seeing your doctor, so it’s important to first understand when you should seek medical help. If you’re experiencing any of the following, consult your GP or make an appointment to speak with one of our Interventional Radiologists:
- Pelvic pain that doesn't go away
- Overly heavy, prolonged or painful periods
- Spotting or bleeding between periods
- Difficulty emptying your bladder
- Unexplained low red blood cell count (anemia)
When it comes to diagnosing, there are a few tests that can be performed:
- Ultrasound – while ultrasounds are useful for detecting abnormal growths in the uterus, they often have trouble differentiating uterine fibroids from other gynecological conditions (such as adenomyosis, which can also be treated by UFE).
- MRI – MRI scans are used to give the full picture in regards to your uterine fibroids. This helps us to determine whether they’re best managed through medication, surgery, or embolisation.
- Hysteroscopy – this procedure uses a small camera to examine the inside of the uterus and look for abnormalities.
How are Fibroids Treated?
There are a number of treatment options available for fibroid sufferers. The first line of treatment is usually conservative management, such as pain control through medication. Many women find this to be effective in managing their symptoms, but it may not benefit all cases, particularly if fibroids are affecting your fertility, or if you have allergies to certain medications.
If medication fails, the size, location, and the number of fibroids are assessed to determine the next course of action, as well as your symptoms, menopausal status, and whether or not you wish to become pregnant in the future.
If it’s seen as in your best interest, it may be recommended that your fibroids be removed surgically (either by myomectomy or hysterectomy), or you can go with a minimally invasive treatment option, such as uterine fibroid embolisation (UFE) to have your fibroids removed without surgery.
Your interventional radiologist will only recommend treatment options that are thought to be best for you as an individual and your unique case.
➡️ Featured Resource: A Complete Guide to Fibroids

Uterine Fibroid Embolisation
Uterine fibroid embolisation (UFE) is a minimally-invasive, image-guided alternative to the invasive surgical procedures used to remove uterine fibroids.
UFE has been used to treat uterine fibroids for over 20 years and has an established role in the management of symptomatic fibroids. It has been shown to reduce symptoms and provide lasting results in up to 95% of cases, and is approved by Medicare.
This is a complex procedure which can only be performed by a specialist interventional radiologist with expertise in the area.
Safe, effective treatments with less pain and quicker recovery.
Ensure you know all your options prior to invasive surgical treatment, schedule a consult with Dr Shaun Quigley.



